Angiograms
and Angioplasty
What is an angiogram?
An angiogram is an imaging technique to visualize blood vessels. Mostly it is used to look at arteries (vessels that transport the blood away from the heart), but at times can also be used to look at veins (vessels that take blood back to the heart). It is helpful to diagnose narrowings or blockages that obstruct the blood flow. Once these are identified they can often be treated at the same time (with an angioplasty, which is explained below)An angiogram. During the angiogram first a needle and then a small, short tube (sheath) is inserted into the vessel, typically in the groin. A special dye (contrast medium) is injected into the blood stream and x-ray pictures are taken as the solution passes along the vessels. The whole procedure lasts approximately one hour, but may take longer if treatment takes place in the same sitting. One of the big advantages is that it can be performed with a local anaesthetic, which means that the patient does not need to go to sleep. The procedure is performed by a vascular surgeon or a specialist interventional radiologist. The picture shows an angiogram of the arteries in the groin.
Preparation for the angiogram
The procedure will have been discussed with the patients in the clinic, when they saw their vascular surgeon. Often at that stage they will have signed the consent form as well. This is to ensure that the procedure and its implications are well understood. In some cases the consent will be signed on the day, when the doctor performing the procedure checks up with the patient briefly beforehand to ensure everything is in order.
Normally patients are admitted to the ward for a few hours in advance to prepare them for the angiogram. On the day it may be possible to eat and drink as normal although this may vary between hospitals. Regular medications should be taken as usual. Blood thinners, especially warfarin, are often stopped before an angiogram. The patients will be instructed by their doctor accordingly beforehand. Also dietary requirements for diabetics, especially when on insulin, will be addressed in advance. The staff will double check some data, for example if you have any allergies or had bad reactions to drugs or other tests. If you have any worries or queries do not be afraid to ask. It is necessary to put on a hospital gown and usually the hair at the groin area needs to be trimmed before the angiogram to help skin cleaning. The procedure will take place in a specialized room, which is either located in the theater tract or the x-ray department. A small drip will be placed into a vein in the arm or hand during the procedure. This may be used to give intravenous fluids. After being positioned on the procedure table, the skin is cleaned in the groin area the patient is covered with sterile drapes. From now on the patient will be asked to lay as still as possible.
During the angiogram
The doctor will inject a local anaesthetic into the skin at the groin numbing the area. Then the fine tube (sheath) is inserted into the vessel. With the help of wires other small long tubes called catheters can be maneuvered through the blood vessels and positioned as desired. The only thing felt during these manipulations is simply a light pressure in the groin. X-ray pictures are taken whilst dye is injected down the catheter into the blood vessels. The dye may cause a hot flush and the feeling of having to pass urine. Both will subside after a few seconds. Multiple injections are necessary to see the full length of the blood vessel and the x-ray machine or the table will be moved in-between them. Once the doctor has identified the problematic parts in the blood vessels, he or she will usually proceed to treat them with a so called angioplasty.
What is an Angioplasty?
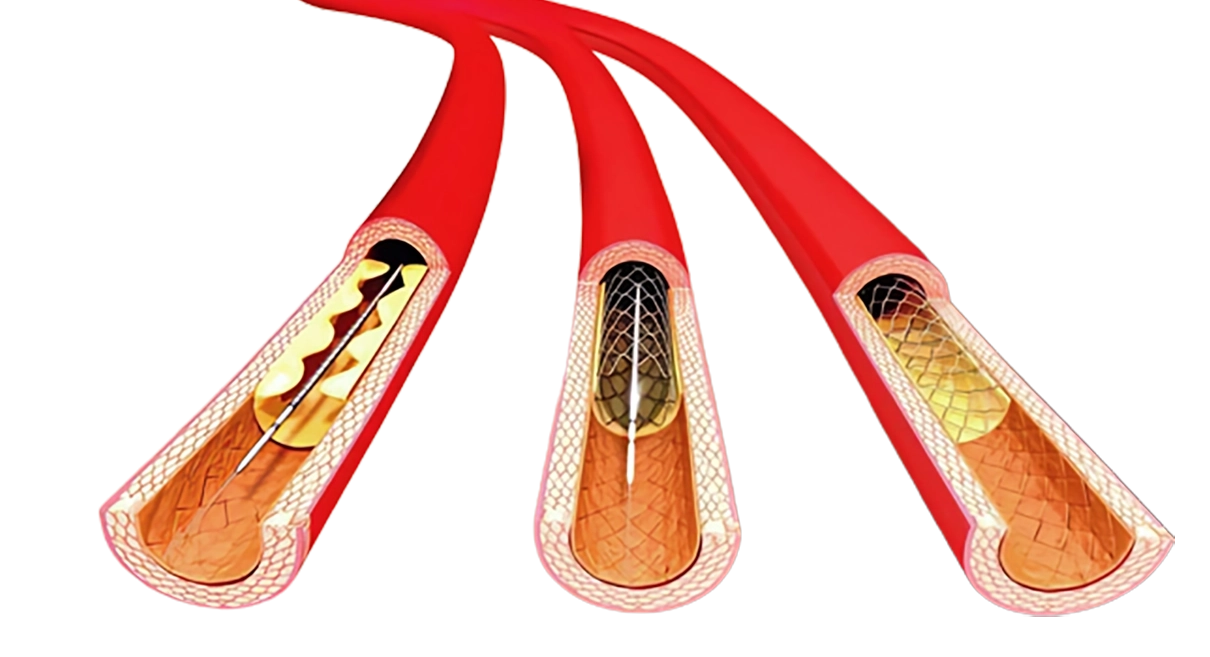
An angioplasty is a minimal invasive (keyhole) technique to treat narrowings or blockages in the vessels that restrict the blood flow. This is done by passing a balloon across the diseased segment and then inflating it. The size of the balloon will match exactly the size of the blood vessel. As a result the plaque will literally be squashed against the vessel wall restoring a good lumen which allows the blood to flow unrestricted. Sometimes a ‘stent’ is inserted afterwards. A stent is a tube made of a special metal mesh and works like a scaffolding to assist keeping the artery open. The picture below shows a pelvic artery before (left) and after (right) an angioplasty of a narrowing in a pelvic artery.
Angioplasty of left common iliac artery
During the angioplasty
The preparations for an angioplasty are the same as for an angiogram. In fact, as explained above, they are often performed at the same time. The doctor will need to use different wires, catheters and balloons during the procedure and a slight pressure may be felt in the groin. An angioplasty obviously takes a little longer than simple angiography and will add to the operation time. A special blood thinning medication will be administered into the drip, so that the blood does not clot off during the procedure. The effects of this medication will wear off after a few hours. Once in position the balloon will be inflated and kept inflated for roughly 90 seconds. During this time a discomfort or painful sensation can be felt whilst the vessel wall is stretched. However, this sensation is usually only mild to moderate and subsides as soon as the balloon is deflated. If a stent needs inserting, this will be done after the stretching. The stent deployment is absolutely pain free.
After the angiogram and/ or angioplasty
When the procedure is done all wires and devices are removed and the sheath is taken out of the vessel. Pressure will be applied to the groin for up to fifteen minutes. Patients are then moved to the recovery area and 2-4 hours of bed rest are necessary to prevent any bleeding from the puncture site. The nursing staff will check the groin, and foot pulses at regular intervals. Depending on whether the procedure was planned as a day case or as an over-night stay the patient will be either allowed to go home or be transferred to the ward. The usual medication may be altered after this procedure and it is important to take any new drugs that are prescribed to ensure an optimal result. Generally a doctor will check on the patient and have a quick chat before discharge.
When going home it is important not to engage in overly physical activity for the day, but rather rest, to ensure that the puncture site in the groin heals up. The next day it is possible to go back to normal. It is important to notify the GP if there should any oozing, swelling, pain or redness develop over the puncture site in the next couple of weeks. There may be restrictions for operating commercial vehicles after surgery, so please check beforehand.
Every patient will be seen again in the clinic by the vascular surgeon to assess the success of the angioplasty and to discuss further proceedings. It is important to remember, that narrowings frequently re-occur or may develop in different areas. Therefore many patients require several future appointments with the surgeon and may even need more procedures and tests in the future.
What are the possible risks?
Generally an angiogram/ angioplasty is very safe. However, as with any operation there are some risks involved. Your surgeon will discuss these with you during the initial consultation and the consent in detail. Here is a brief overview about some of the issues that may be addressed.
Bleeding – as the operation is performed on blood vessels a small amount of bleeding sometimes occurs when the catheter is removed. Before the procedure is finished, the doctor will ensure, by pressing on the artery, that all bleeding has completely stopped. Occasionally this bleeding can cause a small lump around the groin and some bruising in the skin for a few days after the procedure. This is normal and will clear up on its own. Serious bleeding is very uncommon.
False aneurysm – rarely a pulsating lump develops in the groin at the site where the catheter was inserted into the artery. This is because of some continued bleeding from the puncture site into the tissue under the skin after the catheter was removed. The resulting cavity is called a pseudoaneurysm. The lump can usually be seen or felt anytime from directly after the procedure up to two weeks later. Some of these may settle by themselves whilst other may require an additional procedure to fix them. In any case all of these must to be seen by the surgeon.
Pain/Discomfort – local anaesthetic is injected into the skin just before the catheter is placed into the artery. This should take away any severe pain, but it is likely to feel some gentle pushing and pulling during the procedure. The blood vessels themselves do not feel the wires or catheters, however some pain/ discomfort may be experienced during the balloon inflation. Injecting the dye sometimes causes a sensation of warmth, but this usually lasts only a few seconds.
Allergic reactions to the dye – Reactions to modern dyes apart from the sensation of warmth are very uncommon. An extremely small number of patients has an allergy to the dye and may have symptoms. Usually this is a skin rash and itching, but may be in very rare circumstances more severe. The staff are fully trained and equipped to deal with any reaction which may occur.
Damage to blood vessels – this can occur during angioplasty especially if the artery is already badly diseased. The catheter may make a hole in the blood vessel or strip the lining from the blood vessel. Usually these problems can be dealt with at the time of the procedure, but in rare instances open surgery is necessary.
Nerve effects – sometimes the local anaesthetic can numb main nerves in the front of the thigh, causing numbness going down the leg and weakness. This will wear off after an hour or so.
Equipment failure – it is theoretically possible for a catheter, wire or device to break and leave a fragment inside the body. Procedures are available to deal with this eventuality at the time, but occasionally open surgery may be required.
Failure of technique – occasionally it is not possible to perform the angioplasty or the procedure does not show the desired result. In very rare circumstances a failed procedure can actually make the blood flow worse.
Blood clots – despite the blood thinning medication blood clots can form at the angioplasty site within the artery. These can usually be dealt with various techniques, but can sometimes be a problem which can cause the circulation to deteriorate.
Kidney damage – the dye is excreted via the kidneys, which usually deal with this very well. However, especially in patients with pre-existing kidney disease i.e. from diabetes further damage can occur to cells in the kidney. This can lead to deterioration in kidney function. In many cases the kidneys will recover to their pre-operative status, but in few instances the damage persists. Patients with a known kidney condition will be given extra fluids in an intravenous drip before during and after your angiogram, which will reduce the risk of further damage significantly.
How effective is angioplasty?
The effectiveness of angioplasty depends on many factors. It is influenced by general factors like smoking, high blood pressure, high cholesterol, age and other co-existing diseases (i.e. heart or kidneys). It is also influenced by specific factors like the length of the narrowing, its location, the presence of other narrowings or blockages or the size of the vessel. Therefore it is impossible to give an exact prediction on long-term outcomes. Generally it can be said that the smaller the narrowing/ blockage and the bigger the vessel is, the better the outcome will be. It is important to remember, however, that no vascular procedure will last forever. The underlying process (artherosclerosis, ‘hardening of the arteries’) that leads to the formation of the narrowings is a systemic disease, which means that is effects all vessels in the body. The angioplasty will hence address only a certain region, but cannot touch the actual process itself. This is managed with medication and control of risk factors. Hence it is important, that patients continue to take the tablets that were prescribed to them even after a successful angioplasty has made their symptoms disappear. It is also important to break with unhealthy habits, especially smoking as this will significantly influence the long-term success rate as well.